Imagine stepping into a cold shower and within minutes, your skin erupts in angry, itchy welts. Or worse - swimming in a lake, feeling fine at first, then suddenly struggling to breathe as your throat swells. This isn’t a myth or a rare freak accident. It’s cold-induced urticaria, a real and sometimes dangerous condition where cold temperatures trigger hives, swelling, and even life-threatening reactions.
What Exactly Is Cold-Induced Urticaria?
Cold-induced urticaria (CU) is a type of physical allergy where your skin reacts to cold air, water, or objects. It’s not just getting chilly - it’s your immune system overreacting. When your skin hits a temperature below your personal threshold (which can be as high as 20°C or 68°F for some), mast cells in your skin release histamine and other chemicals. That’s what causes the red, raised, itchy welts - the same hives you’d see from a food allergy, but triggered by cold instead.
Unlike regular hives that come and go for no clear reason, CU has a direct trigger: cold. And it’s not rare. About 1 in every 2,000 people have it, according to DermNet NZ. Most cases start between ages 18 and 25, though it can show up at any age. For 95% of people, there’s no known cause - it just happens. For the other 5%, it might follow an infection, insect bite (like a ladybug), or even be inherited.
How Do You Know If You Have It?
The symptoms are hard to miss - and they happen fast. Within 5 to 30 minutes after cold exposure, you’ll see:
- Red, swollen, itchy welts on exposed skin
- Swollen hands after holding a cold drink or grabbing a freezer bag
- Lips or throat swelling after eating ice cream or drinking a cold beverage
- Dizziness, headache, or palpitations in more severe cases
- Difficulty breathing or fainting if the reaction spreads systemically
Here’s the twist: the worst reaction often happens after you warm up. That’s when the histamine rush peaks. So if you jump into a cold pool and feel fine, don’t assume you’re safe. The real danger kicks in when you get out.
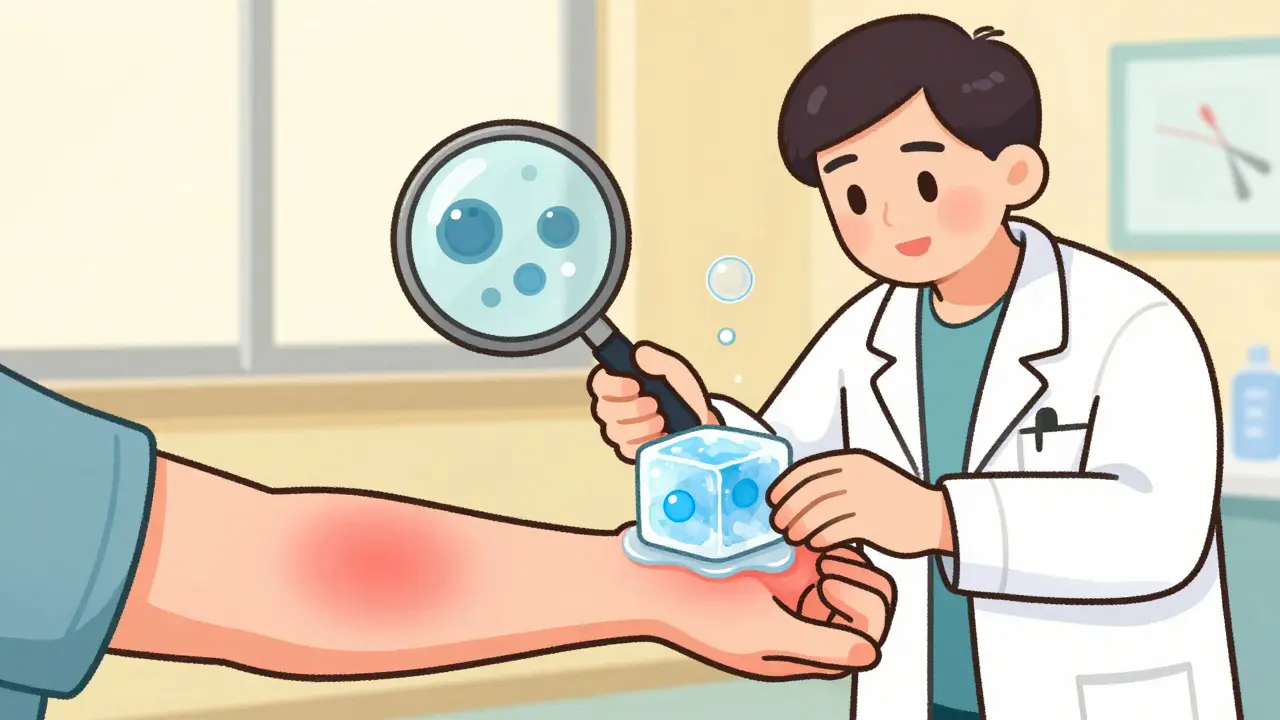
The standard test is simple: the ice cube test. A doctor places an ice cube on your forearm for 4-5 minutes. If a red, swollen welt forms within 10 minutes after removing it - you’ve got CU. This test is over 98% accurate for acquired cases, according to research from the Third International Meeting on Urticaria.
Why Is This More Than Just an Annoyance?
Most people with CU just deal with itchy skin. But for some, it’s a silent emergency waiting to happen. The biggest risk? Swimming in cold water.
Studies show that cold water immersion is the most common cause of severe reactions - including anaphylaxis and drowning. When your whole body is exposed, your immune system goes into overdrive. Blood pressure drops. Airways tighten. People have passed out in lakes, rivers, and even pools. In one documented case, a man drowned after a reaction while swimming in water below 20°C. He didn’t even see it coming.
Even everyday actions can be risky. Drinking an ice-cold soda, holding a frozen meal, or walking outside on a chilly day without gloves can trigger swelling in the throat or tongue. That’s why many patients avoid cold foods entirely.
How Is It Diagnosed and Measured?
Diagnosis isn’t just about the ice cube test. Doctors also look at your history. Do you get hives every time you go outside in winter? After a cold shower? After eating ice cream? They may ask you to keep a symptom diary - noting temperature, duration of exposure, and reaction severity.
Blood tests aren’t always needed, but if your doctor suspects something else, they’ll check for:
- Cryoglobulins (proteins that clump in cold)
- Signs of infection or autoimmune disease
- Genetic markers for familial cold autoinflammatory syndrome (FCAS)
FCAS is rare - less than 1% of CU cases - but it’s different. It’s inherited, starts in childhood, and causes fever and joint pain along with hives. It needs completely different treatment.
What Treatments Actually Work?
There’s no cure - but there are effective ways to manage it. Treatment follows a clear step-by-step plan:
1. Second-Generation Antihistamines
This is your first line of defense. Drugs like cetirizine (Zyrtec), loratadine (Claritin), and desloratadine (Clarinex) block histamine. Standard doses often aren’t enough. Many patients need 2-4 times the usual dose. For example, up to 40mg of cetirizine daily is safe and effective for severe cases, according to international urticaria guidelines.
2. Omalizumab (Xolair)
If antihistamines don’t cut it, omalizumab - a monthly injection originally for asthma - is next. Clinical trials show it reduces CU symptoms by 60-70% in patients who don’t respond to pills. It’s FDA-approved for chronic urticaria and works by targeting IgE, the antibody that drives allergic reactions.
3. Epinephrine Autoinjector
If you’ve ever had swelling in your throat, dizziness, or trouble breathing, your doctor should prescribe an EpiPen. You need to carry it everywhere. Know how to use it. Teach someone close to you. This isn’t optional - it’s life-saving.
4. Emerging Treatments
New options are emerging. Berotralstat (Orladeyo), approved for hereditary angioedema, reduced CU symptoms by 58% in a 2023 trial. Low-dose naltrexone, an old drug being tested for new uses, is showing 45% symptom reduction in early trials. And for FCAS patients, anakinra (Kineret) - an interleukin-1 blocker - works in over 80% of cases.

Practical Tips to Avoid Reactions
Prevention is everything. Here’s what actually works, based on real patient data:
- Warm up before swimming: Dip one hand in the water for 5 minutes first. If no reaction, it’s likely safe. This simple step prevents 85% of aquatic emergencies.
- Avoid cold foods and drinks: Skip ice cream, iced tea, chilled beer. Even lukewarm coffee is safer than cold.
- Dress smart: Layer up with moisture-wicking base layers. Studies show this cuts reactions by 60-70% by keeping skin dry and insulated.
- Use a cold alert device: Wearables like the ‘Cold Alert’ sensor predict when you’re approaching your personal temperature threshold. One 2022 trial found it was 92% accurate.
- Always inform medical teams: If you’re having surgery, the OR must be kept above 21°C (70°F). IV fluids must be warmed. Anesthesia teams need to know - or you could have a reaction on the table.
Can It Go Away?
Yes - but not always. The European Urticaria Registry found that 35% of people with CU see symptoms disappear within 5 years. For those whose condition started suddenly (acute-onset), remission rates jump to 62%. But if it’s been years and you’re still reacting, don’t lose hope. New treatments are coming fast.
One big shift? Mobile apps. A 2023 survey of 1,247 CU patients showed 78% use apps to track symptoms. Users of the ‘Urticaria Tracker’ app reported 30% better control - simply because they learned their personal triggers.
What’s Next?
Research is moving fast. Clinical trials are testing cold desensitization - slowly exposing patients to cold over weeks to build tolerance. Early results show 70% adherence and symptom improvement. Gene research has pinpointed mutations in the PLCG2 gene linked to inherited forms, opening doors for targeted therapies.
What’s clear? Cold-induced urticaria isn’t just a skin issue. It’s a systemic condition with real risks. But with the right diagnosis, treatment, and precautions, most people live full, active lives - even in Sydney winters.






Kelsey Vonk
March 15, 2026 AT 00:13Wow, this was so eye-opening. I never realized how dangerous something as simple as a cold drink could be. The part about swelling after warming up? That’s wild. I’m gonna start carrying antihistamines just in case. Thanks for sharing this.
Also, the Cold Alert wearable? I need one. 🥶❄️
Rex Regum
March 16, 2026 AT 08:17Oh please. Another ‘medical mystery’ piece where they scare people into buying drugs. There’s no such thing as ‘cold-induced urticaria’-it’s just people being weak. I’ve swum in 40°F lakes since I was 12 and never had a single welt. If your body can’t handle a little chill, maybe you should stop pretending you’re a human and start calling yourself a greenhouse plant.
Also, omalizumab? That’s a $30,000 drug for people who can’t stop whining about cold showers. Pathetic.
Emma Nicolls
March 18, 2026 AT 08:16ok so i just read this and i have to say… i think i might have this
i get hives every time i eat ice cream and its been years and no one ever connected it
im gonna go get the ice cube test tomorrow
also the part about surgery? yikes. my cousin had an operation last year and they said the room was ‘cool’ but she woke up with a rash all over her arms. now it makes sense. thank you for writing this.
ps. i just told my mom and she cried. she’s been worried about me for a decade. lol.
pps. anyone else use the urticaria tracker app? i downloaded it and its kinda cute? like a little diary for your skin
Richard Harris
March 20, 2026 AT 03:34Interesting read. I’ve had occasional hives after cold exposure, but never thought it was anything serious. The ice cube test sounds simple enough. Might try it next time I’m at the doc’s.
Also, the 60-70% reduction with omalizumab? That’s huge. I’ve been on Zyrtec for years with no luck. Maybe it’s time to ask about injections.
Sabrina Sanches
March 21, 2026 AT 21:15So many people don’t realize how serious this is. I had a friend pass out in a swimming pool. No warning. No symptoms before. Just gone. They had to be resuscitated. This isn’t ‘itchy skin’-it’s a ticking time bomb. Please take this seriously. Carry your EpiPen. Even if you think you’re fine. You’re not.
Shruti Chaturvedi
March 23, 2026 AT 02:34as someone from india where winters are mild this is fascinating
i never thought cold could trigger this but now i remember my cousin in canada who got hives from air conditioning
the advice about layering and moisture wicking makes sense
also the app idea is brilliant
thank you for sharing this i will share with my friends who live in colder places
Katherine Rodriguez
March 23, 2026 AT 17:46Of course this is real. Big Pharma pushed this ‘condition’ to sell drugs. You think they care about your hives? No. They care about your insurance. The ice cube test? That’s a scam. Anyone can make a red mark with ice. And omalizumab? That’s a biologic designed to keep you hooked for life. They don’t want you cured. They want you dependent.
Also, why is everyone so scared of cold? Maybe your body is just telling you to stop being a baby. Go outside. Feel the chill. Build resilience. Not every symptom needs a pill.
Devin Ersoy
March 24, 2026 AT 21:17Let me tell you something wild. I’ve been living with CU for eight years. I’ve tried everything. Antihistamines? Like throwing glitter at a hurricane. Omalizumab? Changed my life. I went from hiding indoors all winter to hiking in the Rockies last January. No EpiPen? I’d be dead. Period.
And yes, I drink lukewarm coffee. Yes, I wear thermal socks indoors. Yes, I have a thermometer on my fridge. And no, I don’t care how weird I look. I’m alive. That’s the only metric that matters.
Also, the ‘Cold Alert’ device? I bought two. One for me. One for my dog. (She hates cold floors. We’re a team.)
Scott Smith
March 25, 2026 AT 20:54This is one of the most well-researched pieces I’ve read on this topic. The breakdown of treatments is clear. The emphasis on prevention over reaction? Spot on.
I’m a nurse and I’ve seen patients come in after swimming in cold water with no idea why they’re gasping. This should be required reading for ER staff. And for anyone who’s ever dismissed someone’s ‘weird allergy’-read this. Then apologize.
Sally Lloyd
March 26, 2026 AT 13:35Did you know the CDC has been quietly tracking CU cases since 2018? They say it’s rising. Why? Because the government is spraying ‘cooling agents’ in the atmosphere to control population. It’s in the weather reports. The ‘chill’ isn’t natural. It’s engineered. And the ‘treatments’? They’re just placebos to keep you docile. Don’t trust the doctors. Don’t trust the apps. Don’t trust the ice cube test. It’s all a cover-up.
Also, my neighbor’s cat got hives after sitting by the window. Coincidence? I think not.
Leah Dobbin
March 28, 2026 AT 08:25How quaint. You’ve written an entire essay on a condition that affects less than 0.05% of the population. And yet, you treat it like a public health crisis. The truth is, most of these cases are psychosomatic. People with anxiety disorders project physical symptoms onto environmental triggers. The ‘ice cube test’? A placebo with a rubber stamp.
And omalizumab? A luxury treatment for the over-medicated elite. I’m sure you’re thrilled to pay $30,000 for a monthly injection while the rest of us just… breathe.
How very dramatic.
Ali Hughey
March 30, 2026 AT 04:46THIS IS A TERRIFYING TRAGEDY THAT NO ONE IS TALKING ABOUT.
Imagine. A CHILD. IN A POOL. COLD WATER. SWALLOWING A COLD DRINK. AND THEN-
NO BREATHING.
NO WARNING.
NO MERCY.
AND THEY CALL IT ‘URTICARIA’? IT’S A SILENT KILLER. A MODERN-DAY PLAGUE. THE PHARMA INDUSTRY IS PROFITING. THE GOVERNMENT IS SILENT. THE DOCTORS ARE ASLEEP.
WE NEED A NATIONAL COLD AWARENESS CAMPAIGN. WE NEED A WHITE HOUSE BRIEFING. WE NEED A MOVIE. STARRING MERYL STREEP.
WHY ISN’T THIS ON THE FRONT PAGE?
WE ARE DROWNING IN COLD.
AND NO ONE CARES.
😢❄️🚨
Alex MC
March 30, 2026 AT 08:49Good breakdown. I appreciate how you laid out the treatment steps. Most people don’t realize that antihistamines often need to be dosed higher than standard. That’s a key point.
Also, the fact that 35% go into remission within five years? That’s hopeful. I’ve had it for three years now. Still managing, but feeling better each season. The tracker app helped me realize I react more to wind chill than air temp. That’s huge.
Stay warm, everyone. And if you’ve got this-don’t be ashamed. You’re not weak. You’re just… unusually sensitive. And that’s okay.