Opioid Overdose Response Quiz
Opioid Overdose Response Quiz
Time: 2 minWhen someone overdoses on opioids, time isn’t just important - it’s the difference between life and death. Breathing slows down, then stops. Oxygen stops reaching the brain. In just four to six minutes, brain cells start dying. This isn’t a slow decline. It’s a silent, fast-moving crisis. And the people around them - friends, family, strangers - are often the first and only line of defense.
What Happens During an Opioid Overdose?
Opioids, whether prescription painkillers like oxycodone or illicit drugs like heroin and fentanyl, work by attaching to receptors in the brain that control pain and pleasure. But they also attach to receptors that tell your body to breathe. When too much of the drug is in the system, those signals get blocked. Breathing becomes shallow, then stops. The body shuts down. Without oxygen, the heart can’t keep pumping. The brain starts to fail.This isn’t rare. In the U.S., 187 people die from drug overdoses every day. About 81% of those deaths involve opioids. And the biggest driver now? Fentanyl. This synthetic opioid is 50 to 100 times stronger than morphine. A tiny amount - as little as two milligrams - can kill. It’s often mixed into other drugs without the user’s knowledge. A pill sold as Xanax might be fentanyl. A powder labeled as cocaine could be laced with it. You can’t see it. You can’t smell it. But you can die from it.
How to Spot an Opioid Overdose
You don’t need medical training to recognize the signs. There are three clear warning signs that should trigger immediate action:- Unresponsive - No matter how much you shake them or shout their name, they don’t wake up.
- Slow, irregular, or stopped breathing - Look for chest movement. Listen for gasping, snoring, or gurgling sounds. Breathing may be less than once every 10 seconds.
- Pinpoint pupils - Their pupils will shrink to tiny dots, even in low light. (Note: This isn’t always present, so don’t wait for it.)
Other signs include:
- Blue, purple, or gray lips and fingernails
- Cold, clammy skin
- Limp body
- Choking or gurgling noises
- Extreme drowsiness or inability to stay awake
If you see even one of these, assume it’s an overdose. Don’t wait. Don’t hope they’ll wake up on their own. Don’t worry about whether they’re "really" using drugs. Acting fast saves lives.
What to Do in an Emergency
There are three steps - and they must happen in order:- Call 9-1-1 immediately. Tell them it’s a suspected opioid overdose. This gets emergency help on the way.
- Give naloxone if you have it. It’s safe, simple, and works in minutes. Don’t wait for paramedics. Don’t worry about legal trouble - most states have Good Samaritan laws that protect you if you call for help.
- Stay with them until help arrives. Even if they wake up, they can crash again. Naloxone wears off in 30 to 90 minutes. Opioids last longer. They need medical care.
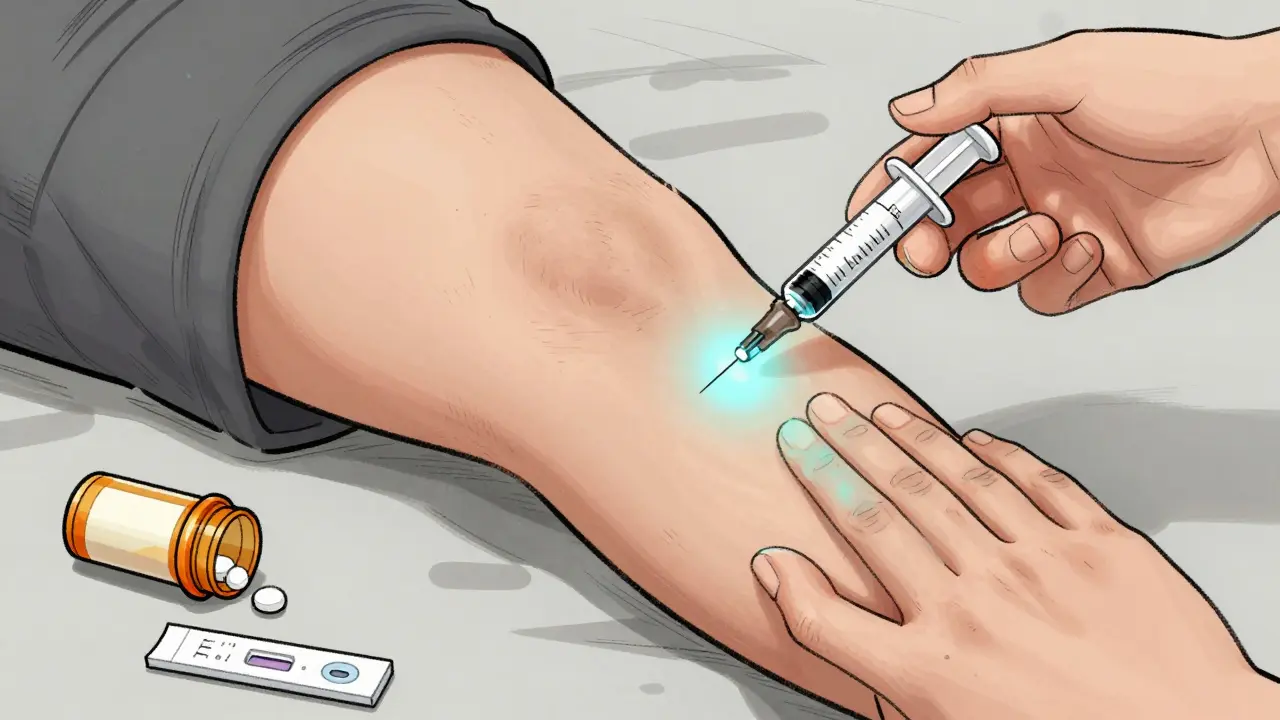
Here’s how to give naloxone:
- Intranasal spray (Narcan): Tilt the person’s head back. Insert the nozzle into one nostril. Press the plunger firmly. You don’t need to aim it - just spray.
- Intramuscular injection: Inject into the thigh, upper arm, or buttock. No special training needed. Follow the instructions on the device.
You can’t overdose someone on naloxone. It won’t hurt someone who hasn’t taken opioids. If you’re unsure, give it anyway. It’s not a gamble - it’s a lifesaver.
What Happens After Naloxone?
Naloxone works fast. Often, the person wakes up within 2 to 5 minutes. They might be confused, angry, or in pain. That’s normal. Opioids were suppressing their body. Now, their system is waking up - and it hurts.But here’s the danger: the overdose can come back. Naloxone’s effects last 30 to 90 minutes. The opioid in their system can last hours. So even if they seem fine, they need to go to the hospital. Paramedics will monitor them. They’ll check for lung damage, heart issues, or brain injury from lack of oxygen.
After the emergency, recovery starts. Many people who survive an overdose don’t get the help they need. That’s why follow-up care is critical. A doctor should check for organ damage. Mental health support should be part of the plan. Medication-assisted treatment (like methadone or buprenorphine) can reduce cravings and prevent future overdoses. And if they’re ready, counseling and peer support make a huge difference.

Where to Get Naloxone
You don’t need a prescription in most places. In 49 states, pharmacists can give out naloxone without a personal prescription. Many pharmacies offer it for free or under $25 - down from over $130 just a few years ago. Community health centers, harm reduction programs, and even some police departments carry it. If you know someone who uses opioids - or if you’re just worried about a friend or family member - get a dose. Keep it in your bag, your car, your jacket pocket. You never know when you’ll need it.Fentanyl test strips are another tool. For less than $1, you can test a small sample of a drug to see if fentanyl is present. It won’t make the drug safe - but it can help someone decide whether to use it, or how much. These strips are legal in most places and available through harm reduction networks.
Why This Matters
Opioid overdoses aren’t just a medical issue. They’re a human one. People don’t overdose because they’re weak. They overdose because drugs are dangerous, unpredictable, and often laced with something deadly. And because the system hasn’t caught up.But we can change that. Every person who learns the signs, carries naloxone, and calls 9-1-1 becomes part of the solution. In communities with naloxone distribution programs, overdose deaths dropped by 14%. That’s not a statistic - that’s real people going home to their families.
You don’t have to be a doctor. You don’t have to be a first responder. You just have to be willing to act. Because in an overdose, seconds count. And sometimes, the only thing standing between someone and death is you.





marjorie arsenault
March 4, 2026 AT 04:59Just carried my first Narcan kit in my purse after reading this. I didn’t think I’d need it… until my cousin’s friend overdosed last month. He woke up after the spray, looked at me like I was crazy, then broke down crying. We don’t talk about this enough. But now? I carry it. Always.
Thanks for the clear steps. Real talk: this could save someone you love.
Deborah Dennis
March 5, 2026 AT 03:22Ugh. Another ‘just carry naloxone’ PSA. People keep using because they’re lazy, irresponsible, and refuse to get help. Why should I risk my time, my money, my energy for someone who won’t even stop? It’s not a public service-it’s enabling.
Levi Viloria
March 6, 2026 AT 13:13I’ve seen this play out in three different towns now. First, it was the guy who sold weed out of his car. Then the girl who took ‘Xanax’ for anxiety. Then my neighbor’s son-thought he was just partying, ended up in a coma for 11 days. Fentanyl doesn’t care who you are. It doesn’t care if you’re ‘responsible.’ It just shows up. And if you’re not ready? You’re not alone. But you better get ready.
Keep the spray in the glovebox. No shame. Just survival.
Richard Elric5111
March 7, 2026 AT 03:22It is, perhaps, an ontological paradox that a substance designed to alleviate suffering has become the most prolific agent of mortality in contemporary American society. The pharmacological mechanism of mu-opioid receptor agonism, while efficacious in pain modulation, exhibits a dangerously narrow therapeutic index when compounded with illicit adulterants. The ethical imperative to distribute naloxone, therefore, is not merely a medical intervention-it is a societal recalibration toward harm reduction as a moral imperative, not a policy afterthought.
Dean Jones
March 8, 2026 AT 13:06Look, I get it. Naloxone saves lives. But let’s not pretend this is a magic bullet. You spray someone awake, they get mad, they walk out of the ER, and six hours later they’re back on the street with a bag of fentanyl-laced powder because the system didn’t give them a single damn thing to hold onto. Treatment centers are full. Therapists are overworked. Recovery programs? Half of them are run by people who’ve never been addicted. We’re treating symptoms while ignoring the rot underneath. The overdose is just the tip of the iceberg-and we’re throwing life jackets at people while the whole damn ship is sinking.
Yes, carry naloxone. But also demand housing. Demand jobs. Demand real mental health care. Or none of this matters in six months.
Zacharia Reda
March 9, 2026 AT 03:02So I got my first Narcan last week. Didn’t know how to use it. Watched a 90-second TikTok. Tried it on my cat. (She was fine. She hissed.)
But seriously-this post made me feel like I could actually do something. Not just scroll and feel bad. Like I could be the reason someone sees tomorrow. That’s not hype. That’s real.
Also-fentanyl test strips are like $1. Buy five. Give one to your weird cousin who says ‘I know what I’m doing.’ They’ll hate you… but they’ll live.
Jeff Card
March 9, 2026 AT 09:16My sister’s been sober for 18 months. She says the hardest part wasn’t quitting. It was realizing how many people didn’t believe she could. They thought she was ‘just another addict.’ But when she OD’d? The guy who’d been her neighbor for years-never talked to her-called 911, gave her Narcan, stayed until the ambulance came. He didn’t know her name. He just saw someone breathing wrong.
That’s the thing. You don’t have to be close to someone to save them. You just have to be awake.
Mike Dubes
March 10, 2026 AT 17:36Just got back from my local pharmacy. Asked for Narcan. The pharmacist handed it to me like I asked for ibuprofen. No questions. No judgment. Just said ‘good for you.’
Went home, put one in my wallet, one in my car, one in my gym bag. My buddy asked why I’m carrying so many. I told him: ‘I don’t want to be the one who had it and didn’t use it.’
And yeah, I spelled ‘Narcan’ wrong in my notes. But I know how to use it. That’s what counts.